Well, no. At least not yet. Plenty of people got sick, but is was mostly run-of-the-mill seasonal flu-style misery. Fevers, aches, pains, head-aches, gastrointestinal woes. In the jargon of the public health set: “mild.” Yet swine flu remains an imminent pandemic and will likely be once all the cases are tallied up.
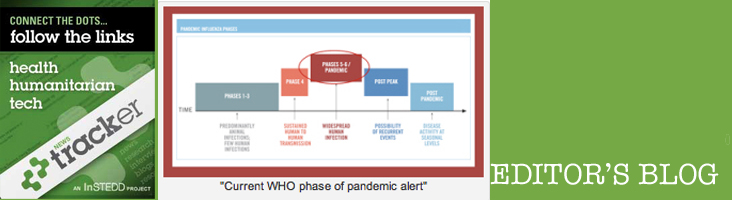
What’s wrong with this scale?
Quite a few things, it turns out. But the biggest complaint from doctors (including my neighbor, a hospital administrator at a major medical center in Chicago) has been its emphasis on viral spread rather than severity of illness.
A possible easy fix:
- Add a new level 6 that factors in virulence along with human-to-human transmission, and bump the current level 6 to a 7.
The scale’s other issues are more subtle. According to the official “WHO phase of pandemic alert” webpage, “pandemic” means “influenza pandemic.” It is as if the SARS scare never happened. In fact, by the WHO’s definition, HIV/AIDS wouldn’t make the cut as a pandemic, despite all evidence to the contrary.
Instead of promoting an approach to biosurveillance designed to track both known and novel pathogens, the WHO’s scale seems oddly specific and limited.
It is even odder considering research the WHO itself has supported to develop cheap rapid diagnostic tests that actually can test for novel pathogens. By a back-of-envelope estimate, 99% of vertebrate viruses have yet to be identified (50,000 vertebrate species, assuming 20 viruses each = 1 million). Since most diseases are zoonotic (meaning they affect multiple species, including humans), such tests are critically important.
Epidemiologist Ian Lipkin, who heads up the Center for Infection and Immunity at the Mailman School of Public Health of Columbia University, which as been working with the WHO, gave a quick overview to three such tests in a recent Pop!Tech lecture: Mass Tag PCR, GreeneChips and High Through-put Sequencing. Each is able to test for dozens of pathogens simultaneously and narrow down candidates. Even if a pathogen hasn’t been seen before, Lipkin’s team can identify its family – what viruses, bacteria or fungi it is related to and how closely – in a matter of hours.
What could be worse than pandemic influenza? How about pandemic rabies? No one is saying the threat is imminent, but the recent emergence of a new strain of the virus in Arizona spreading animal-to-animal through casual contact has researchers more than a little concerned.
Rabies attacks the central nervous system, causing victims to become aggressive, crazy and likely to bite, which is how the virus typically transmits. Fortunatelely, unlike flu where a vaccine must be given prior to infection, a rabies vaccine can be given post-infection. That’s where the good news ends.
The new strain, which mutated from a bat strain, spreads like flu – no bite required – vastly increasing transmission efficiency, especially among social animals such as foxes and raccoons. It has also been seen in skunks. Whether the mutated virus can jump to humans is anybody’s guess, but the fact that it has been observed in foxes means coyotes and dogs are probably at risk. And since foxes, raccoons and skunks have adapted with gusto to the suburban/urban life good life, the opportunity is certainly there.
A wildlife vaccination campaign using an edible vaccine might help contain the spread, but funding is scarce. Howeer, based on limited research, it is clear that the problem has been brewing for a few years, so instead of one small viral fire to put out, there are likely several smoldering across an increasingly large geographic area.
| |